Contributing Authors: Geoff Atkinson, Senior Data Analyst, Management Science Associates, Inc. | Madeline Grant, Business Development Manager, Management Science Associates, Inc. | Paloma Lehfeldt, Director of Medical Education, Vireo Health
One of the promising uses for medical cannabis is treating chronic pain, potentially reducing or replacing prescription opioids and thus reducing the number of overdoses and deaths. Due to the legal status of cannabis and its schedule 1 status on the Controlled Substance Act, there has not been a significant amount of clinical research into its efficacy as a replacement or adjunct therapy for opioids, or its optimal dosing. Unfortunately, due to the lack of research and data there remains uncertainty for patients’ access to pain management and relief through cannabis. The limited research and data availability create uncertainties around patients’ access to cannabis for pain relief. Considering this, Management Science Associates, Inc. (MSA) has taken the initiative to collaborate with cannabis operators such as Vireo Health, aiming to investigate the impact of cannabis consumption on patient health outcomes by utilizing real-world healthcare data. This empirical data is crucial for enhancing our understanding of the complexities surrounding cannabis usage.
MSA and Vireo Health Study
MSA partnered with Vireo Health of Minnesota to complete a first of its kind study for Minnesotan medical patients in the state’s programs. We focused on several hundred customers from eight Vireo dispensaries across Minnesota. Using MSA’s patented de-identification software the data reflected that customers of eight dispensaries in Minnesota reduced their legal opioid usage by an average of 30%. A comprehensive analysis illustrated that these customers, on average, consumed 115 mg of morphine equivalent (MME) per month to their initial cannabis purchase. During the period of cannabis consumption, this figure decreased to 80 MME/month, representing a significant 30% reduction. Notably, opioid prescriptions reverted to higher levels after customers completed their final cannabis purchase. While individual circumstances may necessitate specific medication usage, aggregating data over larger cohort allows for capturing overarching trends.
Once we established, in this particular data set, cannabis may aid in reducing opioid use, we examined additional contributing factors in more detail to determine which patients had the most success. Using MSA’s patented de-identification technology, an individual’s cannabis purchases was matched with their prescription records while maintaining the confidentiality of personal health information. Understanding the connection between cannabis purchasing trends and medical outcomes could be very valuable in making informed decisions about dosing and connecting customers to the products that most effectively meet their particular needs. With the limited clinical research in particular randomized control trials in the United States, there is not nearly as much of this kind of information available for cannabis as there is for more traditional pharmaceuticals. Studies like this are crucial to gather credible data for medical patients to purchase and consume the correct products and dosage.
Continued Results of the MSA and Vireo Health Study
One initial observation is that the impact of cannabis on opioid prescriptions is different for different age groups. Individuals under the age of 45 experienced a 47% decrease in opioid prescriptions, while the 45–64 age group saw an average drop of 35%. Those over the age of 65, who tended to have the highest amount of opioid prescriptions across all three time periods, saw no significant decrease during the time they were purchasing cannabis. There were small differences between men and women. Women used more prescription opioids overall but saw a slightly greater percentage decrease when they began purchasing cannabis.
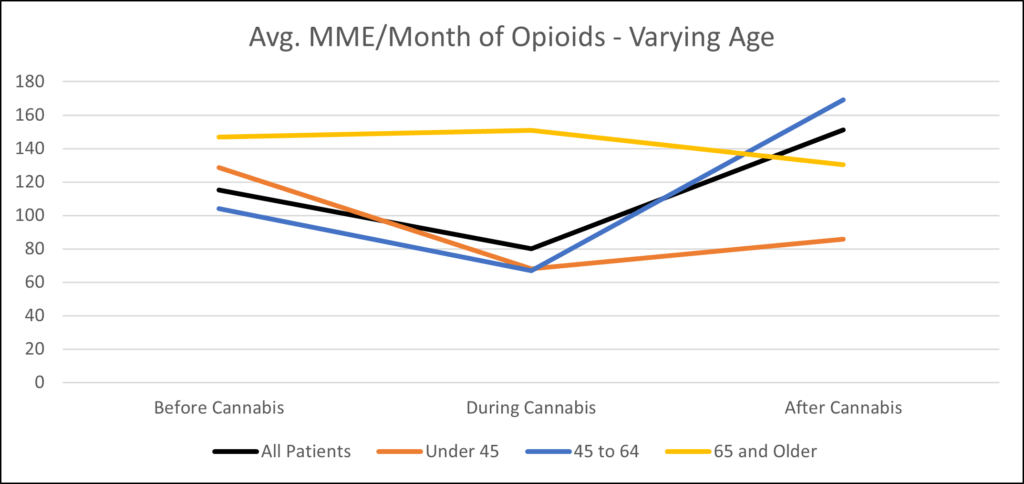
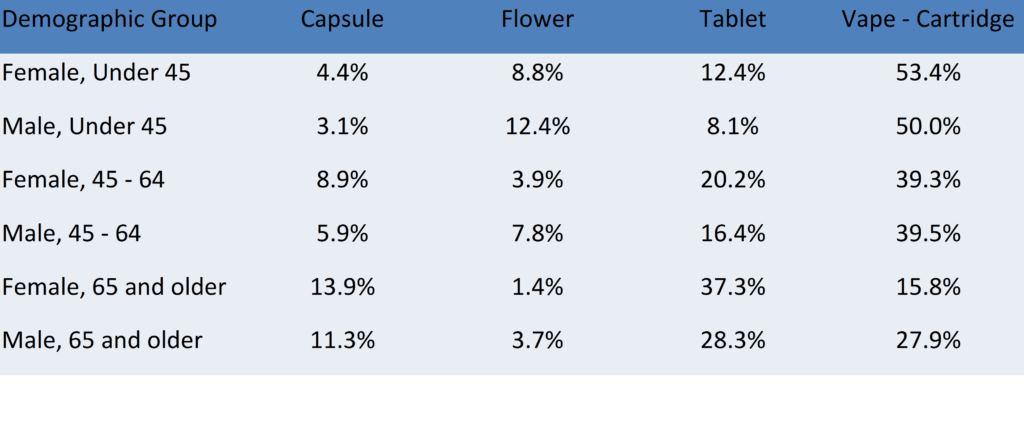
These differences may be related to different demographic groups preferring different forms of cannabis. The table below shows several forms where there were significant differences in percentage of total cannabis spending by age or by gender. For example, younger customers spent more on vape cartridges, and males tended to spend more on flower.
Interestingly, there appears to be no substantial correlation between the total amount of THC purchased and the successful decrease in opioid prescriptions. There was high variation between individuals, but the group of patients who succeeded in reducing their opioid prescriptions purchased an average of 418 mg of THC per month. Those who showed no decrease in opioid prescriptions purchased an average of 563 mg of THC per month. However, those who successfully reduced their opioids did show a preference for products with a high ratio of THC:CBD, spending over 70% of their cannabis budget on products with a ratio of 19:1 or higher.
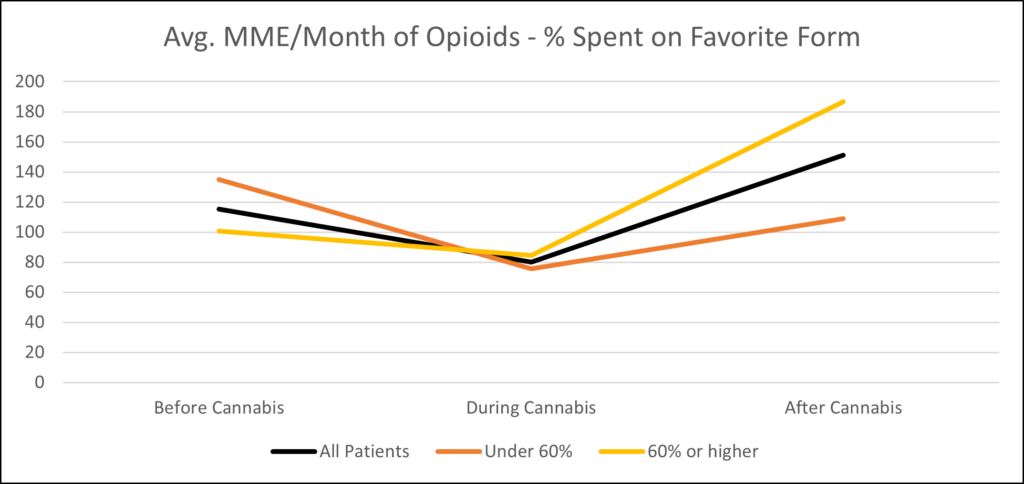
We also examined the connection between different forms of cannabis and patients’ decrease in opioid prescriptions. One interesting way to divide patients is whether they focused on buying one form of cannabis or sampled many different products to find something that would benefit them. Patients who spent over 60% of their total cannabis budget on one form saw an average decrease of 16% in their opioid prescriptions. Patients who were less focused on one form saw an average decrease of 44%. A conflating factor in this analysis is that customers who purchased many different forms of cannabis also tend to have longer periods of cannabis usage. Customers who tried one or two forms of cannabis averaged 136 days between their first and last purchase. Customers who tried three or four forms of cannabis averaged 342 days. Customers who tried five or more forms of cannabis averaged 833 days.
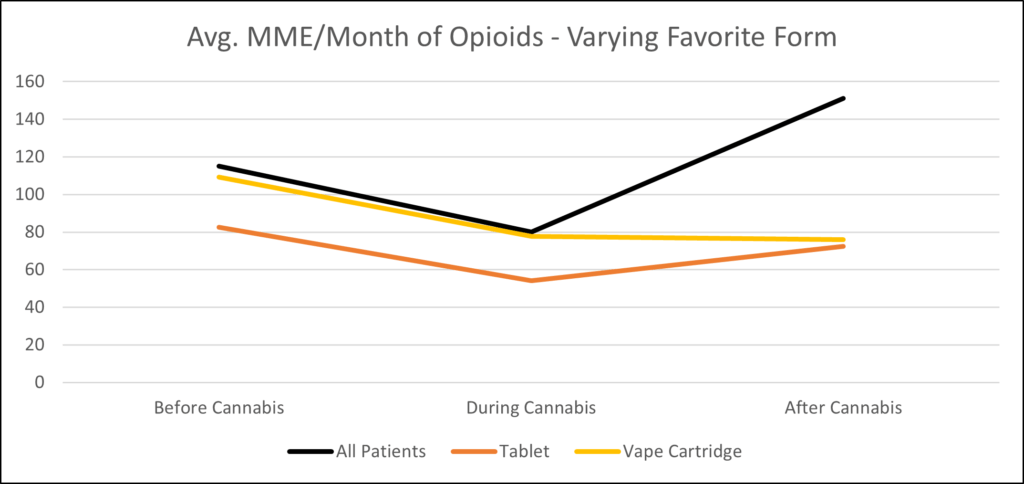
Another way to study the efficacy of particular forms of cannabis is to group patients by their preferred form. For example, customers who spent the majority of their cannabis budget on capsules saw a 63% reduction in opioids while those who preferred tablets saw a 34% decrease. Customers who purchased mostly vape products (the most popular form in these particular dispensaries) saw a 28% decrease, but less rebound towards earlier levels after they stopped purchasing cannabis. Some of these analyses are less statistically significant because of the relatively small number of customers in each group.
Next Steps
While these preliminary findings are intriguing, they underscore the necessity for further research. MSA will continue to look at cannabis customers across multiple states, where different types of products may be available, which might either reinforce our findings, or illuminate some interesting differences between customers in different markets. Looking at more total customers would increase the significance of the findings relating to customers’ preferred forms of cannabis, which would be very helpful in pointing future customers towards the products most likely to help them. MSA will continue to work with cannabis companies, healthcare professionals, advocates, and policymakers across the United States to conduct studies and continue to share reliable data with the cannabis industry.
If you are interested in learning more or getting involved with MSA by being a prominent leader in medical cannabis research, we’d love to hear from you. You can reach out to Madeline Grant at mgrant@msa.com to schedule an introductory call.



Follow NCIA
Newsletter
Facebook
Twitter
LinkedIn
Instagram
–